The information presented in this case study was submitted by the identified provider and reviewed by the Unyte Clinical Team. Modifications to the text have been made solely for the purpose of enhancing comprehension and clarity for the reader’s benefit, and were carefully applied while ensuring the accuracy and integrity of the original submission. Unyte Health makes every effort to use updated terms and inclusive language, this case study retains the author’s original descriptions to be most sensitive to the client’s identity and preferences.
About the Provider
Name: Stacey Christensen
Organization Name: Cook Counseling and Consulting Inc.
Disciplines/credentials: LISW-S (Ohio), LCSW (FL)
Modalities: Safe and Sound Protocol (SSP), Dialectical Behavioral Therapy, Motivational Interviewing, Cognitive Behavioral Therapy, Mindfulness
Client Background
Name: Janine (pseudonym)
Age and Gender: 45-year-old woman
Program Delivered: Safe and Sound Protocol (SSP) Core (Hours 1-5), Balance (Hours 1-2)
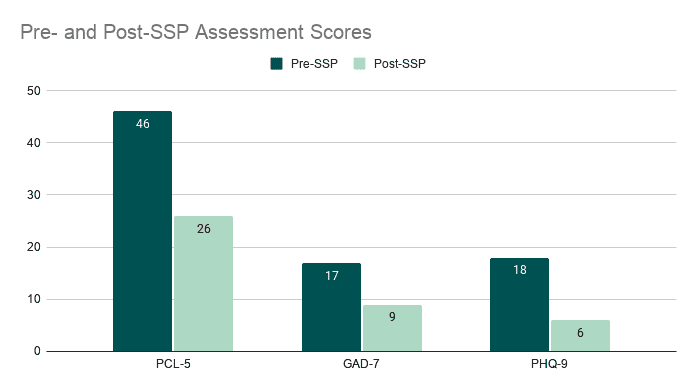
Before starting the Safe and Sound Protocol (SSP), Janine reported experiencing symptoms that made it extremely difficult to function. Her initial pre-assessment scores demonstrated:
- Depression: She scored 18 on the PHQ-9, indicating moderately severe depression.
- Anxiety: Janine scored 17 on the GAD-7, indicating severe anxiety.
- Post-traumatic Stress: She scored 46 on the PCL-5, indicating clinical post-traumatic stress disorder (PTSD) symptoms.
Implementation of the Safe and Sound Protocol (SSP)
Janine started listening to the SSP in person in an office setting. During listening sessions, she participated in activities to support nervous system regulation and engagement, such as:
- Coloring: A soothing, nonverbal outlet for self-expression while helping to maintain a state of calm focus
- Deep breathing exercises: Activates the parasympathetic nervous system, enhancing the ability to remain relaxed and attuned throughout listening
- Quiet listening: Allows the client’s nervous system to process auditory input while being anchored by the provider’s presence
- Journaling: A reflective practice that reinforces self-awareness, tracks nervous system shifts, and supports the integration of therapeutic gains over time
As the provider, Stacey focused on co-regulation, a core principle of the SSP. Stacey’s role was to model and maintain a regulated state, offering consistent co-regulation through tone of voice, body language and responding to Janine’s needs. This helped create the conditions necessary for the SSP to be delivered effectively, ensuring Janine felt supported during the process.
Once Janine had built coping and self-regulation skills in this setting, she transitioned to at-home listening in 5- to 10-minute increments. She continued journaling, recording her thoughts, feelings, bodily sensations and responses after each session, which provided valuable data to track her progress and allowed for ongoing therapeutic adjustment while reinforcing the ability to self-regulate outside the office.
These strategies fostered a calm environment that supported Janine’s capacity for regulation, connection and receptivity to the therapeutic benefits of the SSP.
Response
Janine was consistent with her listening sessions and saw meaningful progress throughout her SSP journey.
Regulation and Emotional Awareness
Early sessions revealed heightened sensitivity to environmental and interpersonal stressors, often resulting in anxious or frustrated mood states. Janine, however, was increasingly able to recognize signs of dysregulation and employ coping strategies. For example, when tension or discomfort arose, she used breathwork or paused to regain a sense of safety and well-being. Over time, she reported feeling calmer, more relaxed, and better able to “talk herself through” heightened responses rather than escalating from “0 to 100.”
Parenting and Family Stress, Interpersonal Dynamics, and Communication
The SSP supported deeper insight into communication patterns within her family relationships, particularly with her husband and mother. Janine identified longstanding tendencies toward avoidance or passive-aggressive communication and began experimenting with alternative approaches, including “I” statements, structured weekly check-ins, and roleplay strategies introduced by Stacey.
Reports of her husband becoming more responsive (for example, completing chores without prompting) reflected positive reinforcement of these skills. Similarly, Janine gained awareness of her mother’s guilt-inducing behaviors and practiced maintaining firmer boundaries, even when this caused short-term discomfort.
Janine’s son’s mental health remained a central source of stress, particularly regarding his intensive outpatient treatments and disclosures of past experiences. Initially, Janine’s responses were dominated by fear and over-responsibility. Through the SSP and therapy, she developed a greater capacity to distinguish between what she could and could not control, apply safety planning strategies, and reduce reactivity in emotionally charged situations. She expressed pride in her son’s progress and her own ability to remain present without escalating her anxiety.
Symptom Reduction and Coping
Self-reported experiences frequently included statements such as “I feel calm,” “I feel better,” and “I feel happy” following sessions, suggesting increased parasympathetic activation and a shift toward autonomic balance. When discomfort arose (initial tension with specific musical protocols), she effectively regulated her state through breathwork or pausing, reflecting improved awareness of internal states and an enhanced ability to modulate physiological arousal.
Toward the end of her SSP journey, she felt an overall sense that her “nervous system is calmer than it was” and noted a significant decrease in reactivity.
Functional Gains
Throughout the SSP, Janine remained oriented, interactive and functionally intact, with no observed or reported suicidal or homicidal ideation or symptoms of psychosis. She demonstrated enhanced insight, improved emotional regulation, and greater self-efficacy in managing relationship challenges and external stressors. Her ability to balance work, family obligations and self-care improved, as evidenced by her recognition of when rest was needed and her willingness to engage in recreational activities and positive social connections.
Significance of Symptom Changes
Janine demonstrated clinically meaningful reductions across all three outcome measures (GAD-7, PCL-5, PHQ-9) over the course of treatment with the SSP combined with psychotherapy.
- Anxiety: Janine’s GAD-7 score decreased by 8 points, shifting from a clinically significant range to mild anxiety symptoms. An 8-point reduction exceeds the minimal clinically significant difference (MCID), indicating a meaningful improvement in daily functioning and distress tolerance. This suggests that she gained increased capacity to regulate anxious arousal and apply coping strategies effectively.
- Post-traumatic Stress: Her PCL-5 score declined by 20 points, moving from the clinical threshold into the subclinical range. A reduction of this magnitude is statistically and clinically significant, reflecting decreased re-experiencing, avoidance, hyperarousal and negative mood/cognition symptoms. This suggests that the SSP may have facilitated greater autonomic regulation, reducing trauma-related reactivity and enhancing the client’s sense of safety and control.
- Depression: Her PHQ-9 score decreased by 12 points, moving symptoms into the mild range. This exceeds the MCID and represents a substantial improvement in mood, energy and motivation. The reduction in depressive symptoms corresponds with the client’s increased engagement in self-care, improved boundary setting, and enhanced relational functioning observed throughout sessions.
These changes reflect cross-diagnostic improvements in emotional regulation, resilience and functional status. Notably, Janine’s movement from clinical to mild or subclinical ranges highlights not only symptom relief but also a shift toward improved quality of life, interpersonal functioning and independence in self-regulation.
From Janine’s perspective:
When I began therapy in February of this year, I came in my rawest, lowest form. My family had just gone through some pretty traumatic events at the beginning of the year, and I was lost.
I’ve always had trouble regulating any strong emotions for as long as I can remember. It has been a struggle I didn’t even realize I was dealing with until my therapist, Stacey, began talking with me about the nervous system, and it just clicked.
SSP has helped me calm my insides. Before I started SSP, when experiencing any intense emotion or situation, I felt like I didn’t have control of what was taking place within my body, and my mind was just off to the races. Since the beginning of SSP, I’ve noticed a significant change in how I am able to process and think about emotions. I’ve learned to slow down my thoughts and calm myself. This has helped me to be more open and honest in my personal relationships. In times of conflict, it has helped me to slow down my thoughts and take a breath before reacting or stepping directly on the “worry train.”
SSP, along with talk therapy, has helped me untangle my insides, which I didn’t even know was possible. In many ways, it has helped me find my voice and become the best version of myself I’ve met so far.
Discussion
Clinical Implications in Light of Polyvagal Theory
Janine’s response to the SSP illustrates the therapeutic potential of auditory interventions grounded in Polyvagal Theory to enhance self-regulation, interpersonal functioning and emotional resilience. According to Dr. Stephen Porges’ polyvagal framework, the autonomic nervous system plays a central role in shaping the perception of safety and in how individuals regulate stress and engage socially.
By modulating neural regulation of the middle ear muscles and optimizing vagal tone, the SSP’s auditory stimulation likely supported greater vagal regulation and increased accessibility of the ventral vagal state, a neurophysiological state associated with calm, connection and openness. This shift enabled Janine to experience safety in her relationships and reduce defensive responses, highlighting the role of the SSP in fostering autonomic balance.
Nervous System Regulation
Throughout the SSP, Janine exhibited a measurable improvement in her capacity for regulation. Early sessions reflected initial hyperarousal, tension and fatigue, which were effectively addressed with co-regulation strategies. As treatment progressed, she increasingly engaged in self-regulation without external scaffolding, reporting feelings of calmness, relaxation and stability after each session. Her ability to pause, reflect and “talk herself through” moments of reactivity aligns with SSP’s aim of improving autonomic flexibility and supporting the transition from defensive states (fight/flight) into regulated states of safety.
Parenting, Caregiving, and Interpersonal and Relational Impact
Janine’s experiences with her son highlight a domain of clinical significance: an increased capacity for the neuroception of safety, allowing her to remain present and supportive without becoming dysregulated. This transformation demonstrates the translation of neuroception into observable behavioral change, as reduced physiological reactivity allowed her to approach parenting challenges with greater openness and flexibility.
Furthermore, improvements in the relationships with her husband and mother suggest that the SSP facilitated nervous system stabilization and created space for shifts in attachment and relational patterns. These gains in communication, boundary-setting and emotional resilience reinforce Polyvagal Theory’s assertion that safety is a prerequisite for authentic social engagement, validating the role of the SSP as a tool to enhance the effectiveness of cognitive-behavioral and relational interventions.
Integration of Remote Client Monitoring
Extending SSP listening beyond the office to short, structured home listening sessions (combined with journaling to encourage reflection and self-awareness) reinforced Janine’s self-regulation skills and provided valuable clinical data for ongoing monitoring and evaluation. Janine’s ability to sustain benefits outside of the clinical setting and generalize her therapeutic gains into her daily life demonstrates the SSP’s adaptability to hybrid care models. These outcomes are consistent with the literature, indicating that the SSP may enhance resilience to environmental and interpersonal stressors.
Overall Clinical Significance
The integration of SSP with psychotherapy produced both subjective and measurable improvements in Janine’s functioning. The magnitude of reduction across all measures suggests that the SSP, combined with psychotherapy, provided direct regulation of the autonomic nervous system and accelerated the therapeutic process by creating a neurophysiological foundation of safety from which cognitive and behavioral interventions (CBT, DBT, communication skills) could be implemented more effectively.
These results suggest that the SSP may serve as a powerful adjunctive intervention that creates the neurophysiological foundation for effective engagement with psychotherapy. Janine’s experience also supports emerging evidence that the SSP, when integrated into psychotherapy, can improve quality of life, reduce anxiety, improve relational functioning, and facilitate long-term resilience through enhanced autonomic regulation.



 © 2026 Unyte Health US Inc.
© 2026 Unyte Health US Inc.