| By Unyte Editorial Team Reviewed by Unyte Clinical Team |
It takes an immense amount of courage for an individual to step into recovery and it’s our job as providers to help provide a safe and encouraging environment.
— Jessica Goldman, LPC resident
Eating disorders are complex conditions that can have a severe impact on your client’s physical and mental health. As providers, it’s important to approach these cases with empathy, a deep understanding of the various types of eating disorders, and a commitment to supporting your clients through the healing journey.
The American Psychological Association defines eating disorders as “characterized by a pathological disturbance of attitudes and behaviors related to food.” While the causes can vary, common contributors include a family history of eating disorders; societal pressures and influences; and anxiety, low self-esteem, or an obsessive personality.
Here is a summary of six eating disorders that can impact clients across the lifespan and common symptoms to look out for.
Anorexia nervosa
Anorexia is characterized by extreme, intentional weight loss, typically through food restriction. Individuals with anorexia demonstrate an intense fear of gaining weight and a distorted body image. Common symptoms include significant weight loss, preoccupation with food, denial of the severity of the weight loss, excessive exercise, and social withdrawal, especially where food is involved.
Bulimia nervosa
Bulimia presents through recurrent episodes of food consumption followed by compensatory behaviors like vomiting, excessive exercise, or laxative use. It can be harder to detect, as individuals with bulimia may be able to maintain a relatively normal weight. If left untreated, however, bulimia can lead to heart and kidney problems, inflammation of the esophagus, dental problems, and nutrient deficiencies. Symptoms include binge eating, self-induced vomiting, preoccupation with body weight, and a distorted body image.
Binge-eating disorder
With binge-eating disorders, individuals will have recurrent episodes of consuming large amounts of food, accompanied by a sense of loss of control. Unlike bulimia, those with binge-eating disorder do not engage in compensatory behaviors. Symptoms include frequent overeating, eating rapidly, discomfort from excessive food intake, and feelings of guilt or shame afterward.
Pica
Pica is an eating disorder defined by the persistent, compulsive consumption of non-food substances. Individuals with pica (typically young children, pregnant people, or those with certain mental health conditions) may ingest items like paper, hair, dirt or clay, which can lead to complications including intestinal blockages or poisoning. Understanding the underlying causes of pica is crucial for developing an effective treatment plan, often involving a multidisciplinary approach with medical and psychological interventions.
Rumination
Rumination disorder describes the repeated regurgitation and re-chewing of food, which may be spat out or re-swallowed. Those with rumination disorder can bring the food back into their mouths without the typical signs of nausea or distress. A collaborative approach between medical professionals and mental health experts is essential for a comprehensive evaluation and the development of therapeutic interventions.
Avoidant/Restrictive Food Intake Disorder (ARFID)
Avoidant/Restrictive Food Intake Disorder (ARFID) manifests as picky eating, reluctance to try new foods, and avoidance of food with specific textures, smells or colors. ARFID is not driven by body image concerns but rather by sensory sensitivities, food aversions, fears (such as a fear of choking) or trauma. Affecting children and adults, those with ARFID experience anxiety when confronted with unfamiliar foods, which can result in a nutrient-deficient diet. Treatment may involve nutritional counseling, trauma-informed exposure therapy, and addressing underlying sensory issues or food-related anxieties.
Identifying an eating disorder and supporting clients
Identifying an eating disorder requires careful evaluation, as symptoms may not always be apparent, although common indicators include weight fluctuations, obsession with body image, changes in eating habits, and social withdrawal. Other physical symptoms can also occur, such as dizziness, fatigue and gastrointestinal issues.
Supporting clients with eating disorders may require a multidisciplinary approach. Firstly, it is important to establish a safe and trusting therapeutic relationship with the client. Creating a space where clients can feel heard and understood without judgment can help set a foundation for the work ahead. Encourage open communication about body image, self-esteem and the emotions underlying their relationship with food.
“It takes an immense amount of courage for an individual to step into recovery and it’s our job as providers to help provide a safe and encouraging environment,” says Jessica Goldman, an LPC resident who has been working with individuals with eating disorders in residential treatment and private practice for three years.
As eating disorders can often be linked to anxiety and feelings of guilt, you may wish to introduce coping mechanisms that promote self-compassion. The Safe and Sound Protocol (SSP) can be a powerful tool used to support your clients in establishing this foundation for awareness, embodiment and resilience.
“When an individual’s nervous system is stuck, they aren’t able to move forward and access that safety,” Jessica adds. “The SSP gives us the ability to help individuals push past their eating disorder thoughts and move deeper into recovery and safety.”
Case study: SSP helps teen in eating disorder facility overcome fear of food
In a case study shared by the Unyte provider community, Wendy Kimelman, LMHC, RN, delivered the Safe and Sound Protocol (SSP) to help 16-year-old Karen, who was in a residential treatment facility for anorexia. Despite conventional therapies, Karen was unsuccessful in increasing her food intake without experiencing severe anxiety that resulted in going back to her restrictive eating behaviors.
To help Karen, Wendy began delivering the SSP for one to two days a week for 30 to 45 minutes per session. During these sessions, Karen would draw or color, sharing that “this is the only time my brain is quiet.”
After completing the SSP, Karen was not the only one to notice a significant change. Prior to the SSP, she struggled to prepare her own meals and snacks without feeling significantly flooded and in fear that she would get too many calories. But after her first meal preparation post-SSP, the floor staff at the facility asked Wendy, “What did you do to that kid?” They shared that Karen was able to prepare her meal without any concerns, and that she seemed relaxed and at ease the whole time.
Further, more real-world evidence demonstrates the efficacy of the Safe and Sound Protocol (SSP) in supporting clients with anxiety.
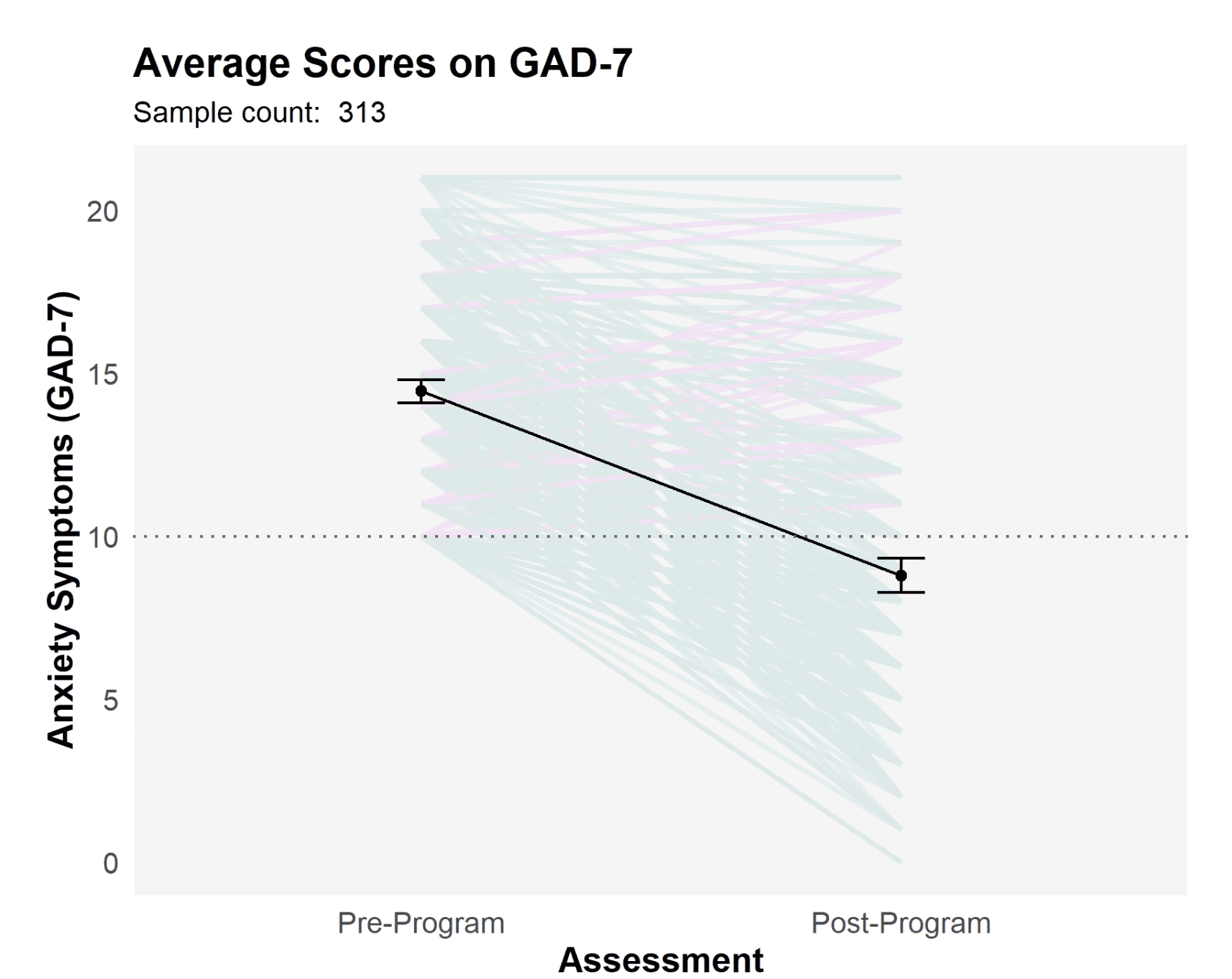
In a real-world sample of 313 clients who initially reported moderate or higher anxiety symptoms on the Generalized Anxiety Disorder (GAD-7) scale, the average score decreased from 14.5 (high severity) to 8.8 (mild severity) after listening to the SSP, representing a 39 percent improvement in symptoms. Additionally, 61 percent of the clients reporting a clinical level of anxiety prior to the SSP transitioned to a non-clinical level after program completion.
Remember that the road to recovery requires a mindful, compassionate and nonjudgmental approach. As providers, your support is key in guiding clients toward a healthier relationship with themselves.




 © 2026 Unyte Health US Inc.
© 2026 Unyte Health US Inc.