| Reviewed by Unyte Clinical Team |
In 2005, the third Monday of January was declared in the media as “Blue Monday.” This claim was based on one psychologist’s formula that determined this date to be the most depressing day of the year.
Many scientists quickly noted a lack of evidence to support this claim, and experts soon uncovered that the psychologist behind “Blue Monday” was commissioned by a now-defunct travel company to determine the best time to sell vacations. (The same psychologist was also asked by an ice cream company to develop a formula for the “happiest day of the year.”)
Although the science behind “Blue Monday” has since been debunked, it may not be uncommon for clients to express feelings of sadness during the colder months. If your client shows symptoms associated with depression, consider talking to them about seasonal affective disorder (SAD).
Symptoms of winter-pattern seasonal affective disorder (SAD)
Seasonal affective disorder (SAD) is a type of depression described by the American Psychological Association as “a mood disorder in which there is a predictable occurrence of major depressive episodes, manic episodes, or both at particular times of the year.” It’s estimated to affect about 5 percent of U.S. adults annually.
Researchers are still exploring the cause of winter-pattern SAD, but studies suggest that it may be linked to reduced levels of serotonin in the brain as a result of shorter daylight hours. Symptoms of SAD can include persistent sadness, hopelessness, irritability, loss of interest in activities, fatigue, concentration difficulties, changes in sleep or appetite, physical discomfort, and thoughts of suicide, according to the National Institute of Mental Health.
Like clockwork, articles are published each year in January with tips and tricks on how to combat “the most depressing day of the year.” While we can dismiss the science behind “Blue Monday,” clients may still be exposed to the concept by friends, colleagues, or social media, and want to talk about it. Providers should take care to address their concerns, especially if they show symptoms related to SAD.
Supporting clients with the Safe and Sound Protocol (SSP)
The Safe and Sound Protocol (SSP) may be an option as you look for ways to help your clients, backed by real-world evidence demonstrating its efficacy in supporting individuals experiencing depression-related symptoms.
In a real-world data sample from Unyte providers, 208 clients reported at least moderate symptoms of depression on the Patient Health Questionnaire (PHQ-9) before starting the SSP Core program. Following the completion of the SSP Core, the average score on the PHQ-9 decreased from 15.2 (high severity) to 9.8 (mild severity), translating to a 36-percent improvement in symptoms.
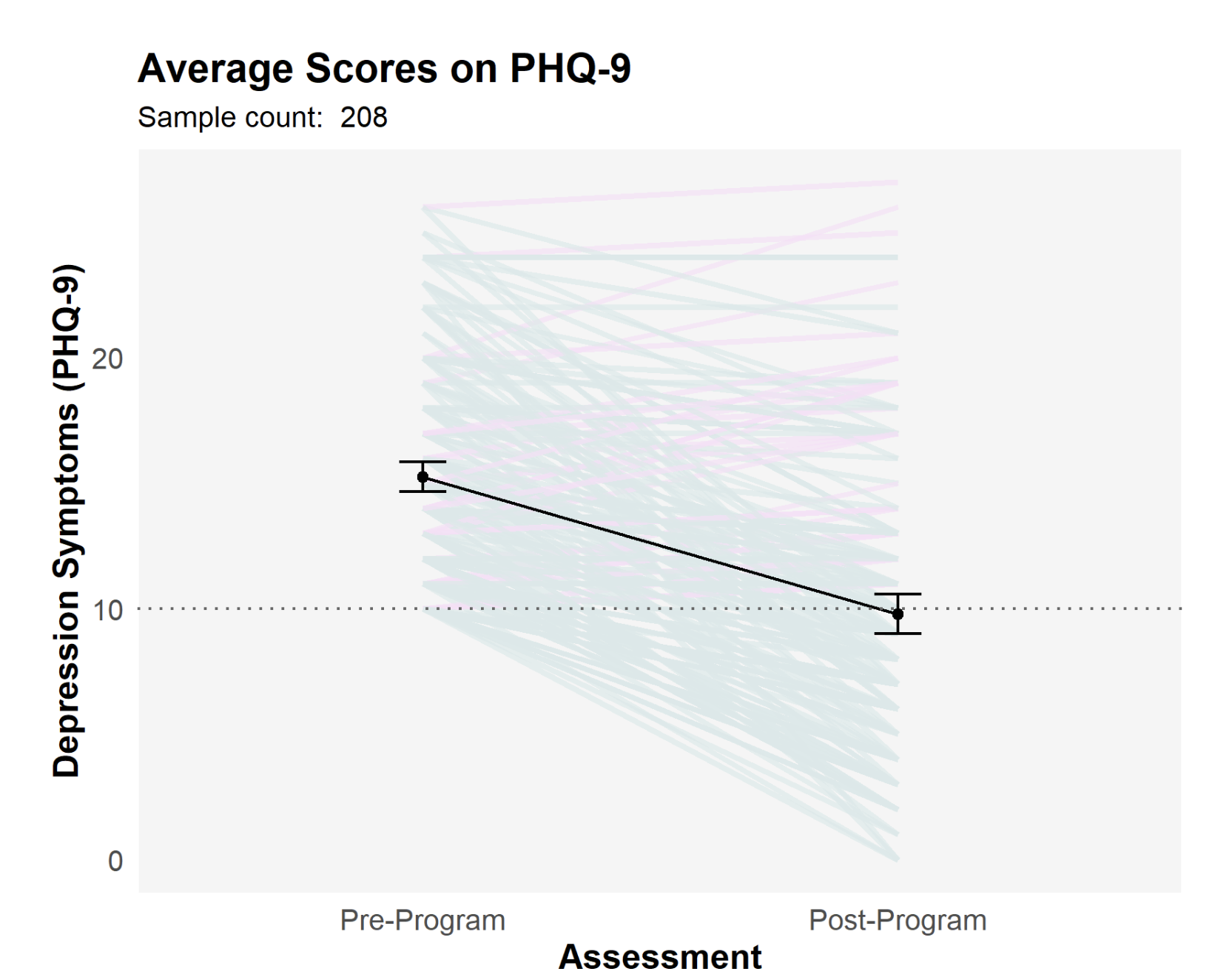
Another significant result was that 54 percent of the clients moved from a clinical level of depression to non-clinical (a score less than 10). In a separate case study submitted by an SSP Provider, a 59-year-old client who had experienced depression for 31 years reported no longer waking up with feelings of dread after the SSP, explaining that her lingering depression “slid away,” and that she felt that she was in a ventral state for the first time in decades, possibly for the first time ever.
“[She] still can’t believe how she feels when she wakes up after being past one month of completion of the SSP Core pathway,” said Terri Bernath, SSP Provider.
Additionally, real-world evidence shows positive results post-SSP in clients presenting with anxiety, trauma, and psychosocial challenges, further demonstrating the potential benefits of the SSP.
Continue your learning
The SSP is a listening therapy developed by Dr. Stephen Porges based on decades of research known as Polyvagal Theory. The program uses five hours of music that has been specially filtered through an algorithm designed to help regulate the autonomic nervous system.
As a non-invasive listening therapy, the SSP is very low risk, especially compared to vagus nerve stimulation (VNS) devices or pharmaceutical interventions. No adverse events have been reported by participants in any of the clinical trials. In one study, SSP participants reported mild, temporary side effects including headache, sleeplessness and fatigue, which did not limit or disrupt program completion” (Kawai et al., 2023).




 © 2026 Unyte Health US Inc.
© 2026 Unyte Health US Inc.