| By Susanna Coss Reviewed by Rebecca Knowles, OTD, OTR/L, RYT |
Earlier this year, Japanese researcher Hiroki Kawai and his team at Okayama University completed an exploratory pilot study evaluating the effectiveness of the Safe and Sound Protocol (SSP) in adults with autism (Kawai et al., 2023). In this study, published in the International Journal of Environmental Research and Public Health, the SSP was delivered to six participants over five consecutive days for 60 minutes each day. Features of social communication, cognition, sensory processing, and emotional and behavioral regulation were assessed before, one hour after, and one month after completion of the SSP Core program.
Of these features, the most significant improvements were observed in social awareness. Social awareness refers to an individual’s capacity to perceive social cues and understand the perspectives and intentions of others in social situations. It is largely influenced by sensory components, such as listening, sight, and touch (Goleman and Davidson, 2017).
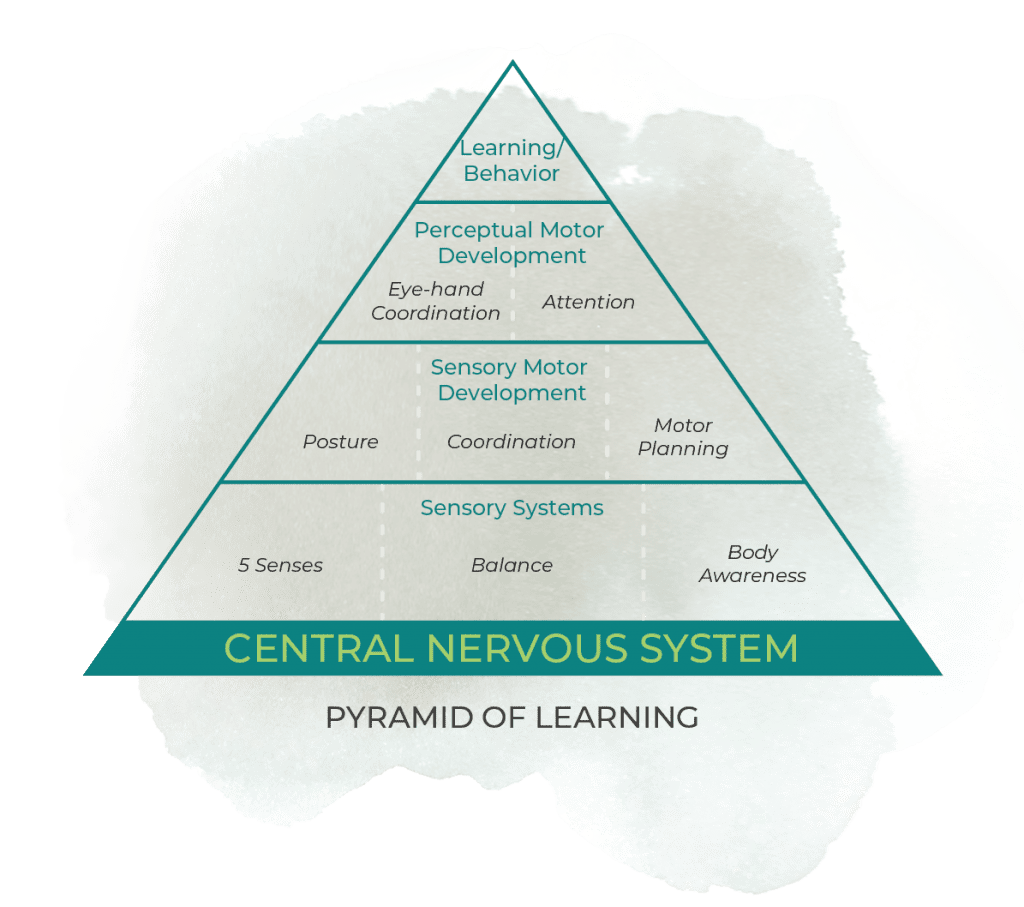
Speaking with Unyte, Hiroki said social awareness stood out from the other features measured, as it relies on the use of the senses to understand and relate to others, whereas the other categories more heavily involve movement and thinking skills. In nervous system development, the sensory systems develop first and set a foundation for higher brain functions, such as communication and behavior (Williams and Shellenberger, 1996). The observed change in social awareness aligns with the way the SSP works — by gently creating bottom-up changes that prime the nervous system for further growth. Some SSP providers experimenting with additional rounds of the SSP noted enhancements in their clients’ communication and learning skills as the SSP retuned each level of the nervous system, reflective of developmental order.
Social awareness improvements also correlated with a reduction in state anxiety and feelings of anxiety triggered by a specific situation or stimulus (Smith and Johnson, 2018). This again highlights the SSP’s ability to retune the sensory systems to respond more adaptively to external stressors.
Furthermore, narrative reports from participants and their family members included in the study help us better understand the effects of SSP in the real world beyond what assessment measures can capture. These personal accounts highlighted enhancements in responsiveness, awareness, sensory sensitivity management and vocal volume control. One participant, who had suffered from insomnia since childhood, achieved the remarkable milestone of sleeping through the night after the SSP. Additionally, the majority of participants expressed a desire for additional rounds of the SSP, indicating their positive experiences and potential for continued progress.
Evidence for the SSP was first established in 2013 and 2014 in two compelling clinical trials on children with autism that positioned the SSP as a promising therapeutic intervention for this population (Porges et al., 2013; Porges et al., 2014). Since then, further studies have explored the impact of the SSP in reducing symptoms of depression; Functional Neurological Disorder (FND), as published in the Harvard Review of Psychiatry; and supporting adults with autism (Burns, 2022; Kawai et al., 2023; Rajabalee et al., 2022).
As we have learned from the Unyte provider community, tailoring the SSP listening experience to the needs of an individual’s unique nervous system and cultivating a supportive environment of safety helps optimize its benefits. Although the need to keep the experience for all participants uniform within a research setting limits the researcher from exploring these aspects fully, the SSP still demonstrated positive shifts even without an individualized delivery model.
This is yet another study that speaks to the transformative potential of the SSP and how it works to gently repattern the nervous system to safety, demonstrating its ability to influence the nervous system from the bottom up and helping us look to future applications and populations that may benefit from the SSP.

Discover the Safe and Sound Protocol
Developed by Dr. Stephen Porges, the SSP is a non-invasive acoustic vagus nerve stimulator that helps clients connect with themselves, others, and the world from a foundation of physiological safety.
References
Burns, S. (2022). HRV measurement not predictive of depression symptoms or improvement: a case report. Cogent Psychology, 9(1). https://doi.org/10.1080/23311908.2022.2080318
Goleman, D., & Davidson, R. J. (2017). The role of attention in social awareness. In R. J. Davidson & A. Fox (Eds.), The Oxford Handbook of Social Neuroscience (pp. 229-245). Oxford University Press.
Kawai, H., Kishimoto, M., Okahisa, Y., Sakamoto, S., Terada, S., & Takaki, M. (2023). Initial Outcomes of the Safe and Sound Protocol on patients with adult autism Spectrum Disorder: Exploratory Pilot Study. International Journal of Environmental Research and Public Health, 20(6), 4862. https://doi.org/10.3390/ijerph20064862
Porges, S. W., Bazhenova, O. V., Bal, E., Carlson, N., Sorokin, Y., Heilman, K. J., Cook, E. H., & Lewis, G. F. (2014). Reducing auditory hypersensitivities in autistic spectrum disorder: preliminary findings evaluating the listening project protocol. Frontiers in pediatrics, 2, 80. https://doi.org/10.3389/fped.2014.00080
Porges, S. W., Macellaio, M., Stanfill, S. D., McCue, K., Lewis, G. F., Harden, E. R., Handelman, M., Denver, J., Bazhenova, O. V., & Heilman, K. J. (2013). Respiratory sinus arrhythmia and auditory processing in autism: modifiable deficits of an integrated social engagement system?. International journal of psychophysiology: official journal of the International Organization of Psychophysiology, 88(3), 261–270. https://doi.org/10.1016/j.ijpsycho.2012.11.009
Rajabalee, N., Kozlowska, K., Lee, S. Y., Savage, B., Hawkes, C., Siciliano, D., Porges, S. W., Pick, S., & Torbey, S. (2022). Neuromodulation using computer-altered music to treat a ten-year-old child unresponsive to standard interventions for functional neurological disorder. Harvard Review of Psychiatry, 30(5), 303–316. https://doi.org/10.1097/HRP.0000000000000341
Smith, J. K., & Johnson, A. B. (2018). Understanding state anxiety: A comprehensive review of theoretical, empirical, and clinical aspects. Journal of Anxiety Disorders, 42, 44-58.
Williams, M.S., & Shellenberger S. (1996). How does your engine run? Leader’s guide to the alert program for self regulation. Albuquerque, NM: TherapyWorks.



 © 2026 Unyte Health US Inc.
© 2026 Unyte Health US Inc.